Pelvic Exam
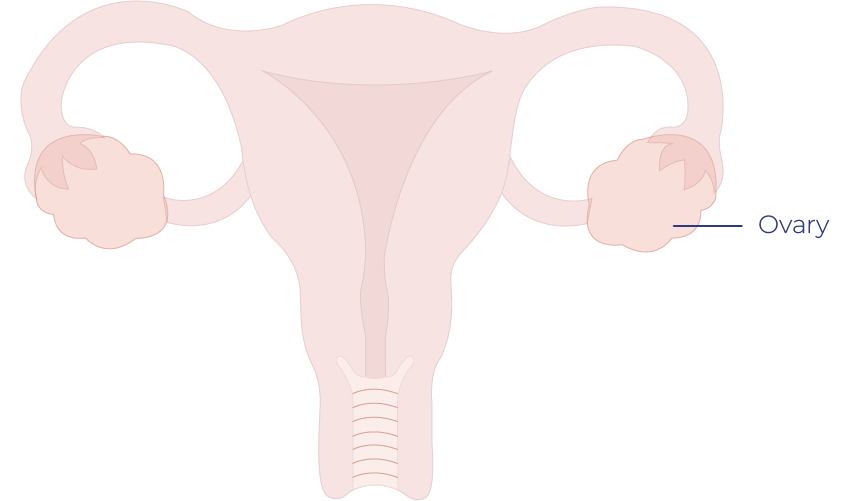
A doctor or nurse examines your vulva and your internal reproductive organs — your vagina, cervix, ovaries, fallopian tubes, and uterus. This exam requires the doctor to place one or two fingers into the vagina and another over the abdomen to feel the size, shape, and position of the ovaries and uterus. Ovarian cancer is rarely detected in a pelvic exam and usually in an advanced stage if it is.
Transvaginal Ultrasound
A transvaginal ultrasound is a test used to examine a woman’s reproductive organs and bladder, and can often reveal if there are masses or irregularities on the surface of the ovaries and within cysts that form within the ovaries. To administer the test, the doctor inserts a probe into the vagina. The probe sends off sound waves which reflect off body structures. The waves are then received by a computer that turns them into a picture. An ultrasound alone is not an accurate way to screen for ovarian cancer.
The CA-125 Blood Test
Measures the amount of a protein called CA-125 in the blood. CA-125 is a substance in the blood that can increase when a cancerous tumour is present; this protein is produced by ovarian cancer cells and is elevated in more than 80 percent of those with advanced ovarian cancers and in 50 percent of those with early-stage cancers.
It is not a reliable early detection test for ovarian cancer. In about 20 percent of advanced stage ovarian cancer cases and 50 percent of early stage cases, the CA-125 is not elevated even though ovarian cancer is present. As a result, doctors generally use the CA-125 blood test in combination with a transvaginal ultrasound. Because CA-125 misses half of early cancers and can be elevated by non cancerous conditions such as endometriosis and pelvic inflammatory disease.