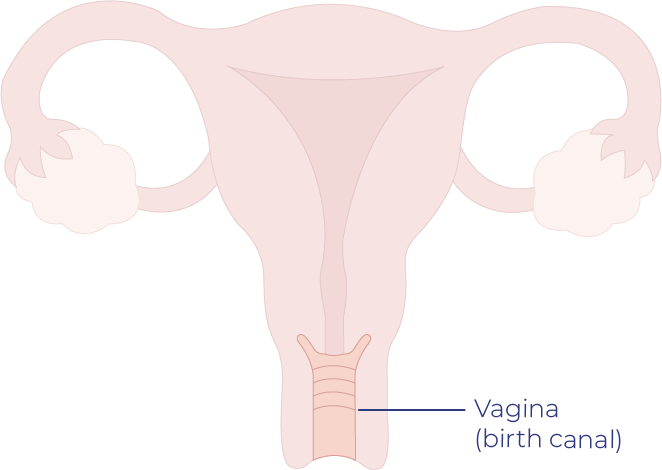
Vaginal cancer is cancer that starts in and affects the vagina.
Vaginal Cancer
See your GP or a gynaecologist if you notice any changes or experience any persistent symptoms that worry you. Any changes should ALWAYS be investigated.
Vaginal Cancer – Risk Factors
What causes vaginal cancer?
- People who have HPV (human papillomavirus), a sexually transmitted disease that can increase the risk of several cancers of the reproductive organs, including vaginal and cervical cancer. In most, an HPV infection will go away on its own, but for some, it causes cell changes that increase their risk of cancer.
- People who have a history of precancerous vaginal conditions. Precancerous cells in the vagina are called vaginal intraepithelial neoplasia (VAIN). These cells are not malignant, but are different from normal cells. The majority of people who develop VAIN do not go on to develop cancer, but some do. VAIN is caused by HPV infection.
- People who have had a hysterectomy (removal of the uterus), because this increases the risk of VAIN.
- People who have been treated for cervical cancer or precancerous cervical conditions
- People whose mothers took DES (diethylstilbestrol) to prevent miscarriage, a drug that was often prescribed in the 1950s, when they were pregnant. These people are at risk for a particular type of vaginal cancer, adenocarcinoma.
- Smoking doubles the risk of developing vaginal cancer.
- Age. The average vaginal cancer patient is diagnosed after the age of 60, and a person’s risk of developing it increases as they get older.
PLEASE NOTE: Vaginal cancer can affect anyone with a vagina at any age.
Vaginal Cancer – Diagnosis
Tests to diagnose vaginal cancer may include:
Physical Examination
It is standard practice for your doctor to examine your vagina, groin and pelvic area. A nurse may be present during the examination, and you are allowed to have a support person of your choosing present.
Cervical Screening Test
You may undergo a cervical screening test to check the cells inside the vagina and cervix as part of the physical examination. Results may show early cell changes in the vaginal lining.
Colposcopy and Biopsy
During the examination, your doctor may use a magnifying instrument called a colposcope to look at your vagina, cervix and vulva. Your doctor may also take a tissue sample (called a biopsy) to check for cell abnormalities.
Further Tests
If the tests described above show that you have vaginal cancer, further tests may be needed to find out if the cancer cells have spread to other parts of the body. These tests may include a blood test, chest X-ray, cystoscopy, proctoscopy, and CT and MRI scans.
Vaginal Cancer – Treatment
Staging
Based on the results of the tests, your doctor will tell you the stage of the cancer. Staging describes the size of the cancer and if and how far it has spread beyond the vagina.
Your doctor may also tell you the grade of the cancer cells. This gives you an idea of how quickly the cancer may develop.
Knowing the stage and grade of the cancer helps your medical team decide on the most appropriate treatment. Treatment may involve radiotherapy, surgery and/or chemotherapy.
Radiation Therapy
Radiation therapy (also known as radiotherapy) is a common treatment for vaginal cancer that uses radiation, such as X-rays, to kill or damage cancer cells. Radiotherapy can also be used to control symptoms of advanced cancer. This is called palliative radiotherapy.
Surgery
The cancer may need to be removed with an operation. Surgery will aim to remove all of the cancer along with some of the surrounding healthy tissue (called a margin). This helps reduce the risk of the cancer coming back. Some lymph nodes in your pelvis may also be removed.
Chemotherapy
Chemotherapy uses drugs to kill or slow the growth of cancer cells. It is usually given if the vaginal cancer is advanced or returns after treatment, and may be combined with surgery or radiotherapy.
Chemotherapy may be given as tablets or by injection into a vein (intravenously). You will usually have a number of treatment sessions, followed by a break.
Don’t feel silly going to the doctor – it’s your body, you know it better than anyone else!
I believe I have these symptoms – what next?
Please make an appointment to see your GP
Write a list of the symptoms that are present and any other concerns to take with you to your GP or gynaecologist
You should tell them about any changes to your body that you have noticed. You should tell them if you or anybody in your family has had cancer or been tested for genetic faults.
Symptoms can often be attributed to other conditions such as irritable bowel, indigestion, and stress – common complaints that GPs are attending to. It’s extremely important to note that if you feel your symptoms are not the ordinary for you, are persistent and have gotten worse that you advocate for your health.
1. Take a list of the symptoms that are present- give your GP as much information as you can.
2. Consider your whānau/family history and discuss this with your doctor. Call whānau/family and try to get a gauge on what cancers if any have been present. Please note that a gynaecological cancer can be present even if there has been no whānau/family history of one.
3. Ask your GP for a second opinion or referral to a specialist
4. You are by rights allowed to take someone along with you to your GP and specialist visits for moral support, it’s great to have someone there especially when being given a lot of new information.
5. NEVER feel silly or like you are overreacting by seeking the advice of a medical professional YOU know your body better than anyone else.