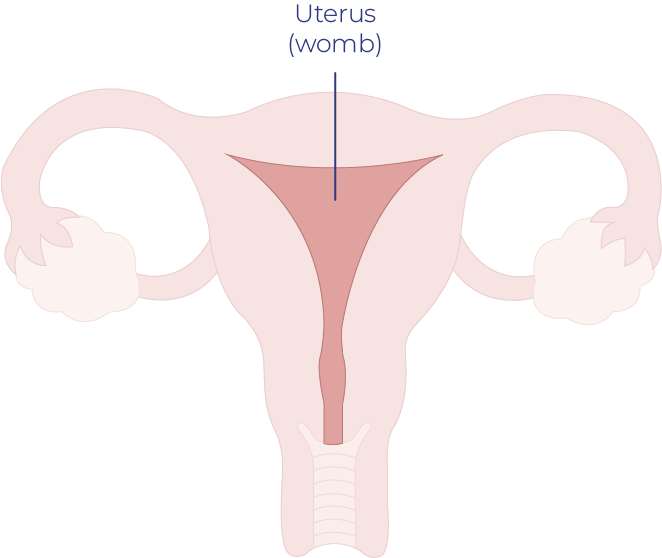
The most common symptom of uterine cancer is abnormal vaginal bleeding. This includes a change in menstruation: heavier periods, periods that last longer or periods that occur more often than normal, bleeding between periods or bleeding after menopause, unusual vaginal discharge (this can be a watery, pink or dark bloody discharge).
Uterine Cancer
See your GP or a gynaecologist if you notice any changes or experience any persistent symptoms that worry you. Any changes should ALWAYS be investigated.
Uterine Cancer – Risk Factors
There is no definitive way to know for sure if you will get uterine cancer. Some people get it without being at high risk. However there are several factors that may increase the possibility that you will develop uterine cancer, including:
- Age. People over the age of 50 are more at risk, BUT this cancer does not discriminate and people of all ages can develop uterine cancer.
- Being overweight or obese. Fat tissues tend to produce higher levels of estrogen, particularly after menopause, which increases the endometrial cancer risk for older people.
- Having been diagnosed with breast or ovarian cancer in the past
- Having been diagnosed with endometrial hyperplasia in the past
- Treatment with radiation therapy to the pelvis to treat another cancer
- Taking estrogen medication by itself (without progesterone) for hormone replacement during menopause.
- Taking tamoxifen, a drug used to treat certain types of breast cancer. People who are treated with the breast cancer drug tamoxifen have an increased risk of developing this disease.
- Have close family members who have had uterine, colon, or ovarian cancer.
- Things that affect hormone levels, for example taking estrogen medication after menopause, birth control pills, or tamoxifen
- Increased number of menstrual cycles. People who have had more menstrual cycles in their lifetime have an increased endometrial cancer risk. This includes those who started their periods before age 12 and who went through menopause after age 50.
- No prior pregnancies. Researchers are investigating why pregnancy seems to reduce the risk of endometrial cancer. During pregnancy, a person’s hormonal balance shifts, with her body producing more progesterone and less estrogen.
- Irregular menstrual cycles and infertility also may cause imbalances in estrogen and progesterone levels, which may increase the risk of endometrial cancer.
If one or more of the above are true for you, it does not mean you will get uterine cancer, but you should speak with your doctor to see if he or she recommends more frequent screening or monitoring.
Never feel silly about going to talk to a health professional about any concerns you have around your health. It’s your body you know it better than anyone else! What’s normal for one person does not mean normal for the next.
Uterine Cancer – Treatment
Uterine cancer is treated by one or a combination of treatments including surgery, radiation therapy, chemotherapy, and hormone therapy.
Combinations of treatments are often recommended, but they depend on the stage and characteristics of the cancer.
Uterine Cancer – Stages
All cancers are given a ‘stage’. The stage indicates the size of the tumour and the extent of its spread throughout the body. Uterine cancer may be given the following stages:
Stage I
Stage 1 cancers are the easiest to treat.
1A means that the cancer may have grown into the muscle wall (myometrium) of the uterus, but no more than halfway.
1B means the cancer has grown halfway or more into the muscle wall of the uterus.
Stage II – Cancer of the Uterus
This means the cancer has spread to the cervix.
Stage III – Cancer of the Uterus
This stage means the cancer has spread further. There are three categories of stage 3 uterine cancer:
3A means the cancer has grown into the ovaries.
3B means the cancer has spread into the vagina or into the tissues surrounding the uterus.
3C means the cancer has spread to nearby lymph glands.
Stage IV
This stage means that the cancer has spread to another body organ. There are two categories of stage 4 cancer of the uterus:
4A means the cancer has spread to the bowel and bladder.
4B means the cancer has spread to other organs that are further away, such as lungs, liver, bones or brain.
I believe I have these symptoms – what next?
Please make an appointment to see your GP
Write a list of the symptoms that are present and any other concerns to take with you to your GP or gynaecologist
You should tell them about any changes to your body that you have noticed. You should tell them if you or anybody in your family has had cancer or been tested for genetic faults.
Symptoms can often be attributed to other conditions such as irritable bowel, indigestion, and stress – common complaints that GPs are attending to. It’s extremely important to note that if you feel your symptoms are not the ordinary for you, are persistent and have gotten worse that you advocate for your health.
1. Take a list of the symptoms that are present- give your GP as much information as you can.
2. Consider your whānau/family history and discuss this with your doctor. Call whānau/family and try to get a gauge on what cancers if any have been present. Please note that a gynaecological cancer can be present even if there has been no whānau/family history of one.
3. Ask your GP for a second opinion or referral to a specialist
4. You are by rights allowed to take someone along with you to your GP and specialist visits for moral support, it’s great to have someone there especially when being given a lot of new information.
5. NEVER feel silly or like you are overreacting by seeking the advice of a medical professional YOU know your body better than anyone else.